
Supporting safer community palliative care with Palliate
Improving the access and quality of training and support for lay carers to administer subcutaneous end-of-life medications in the home.
What is the problem we are solving?
It is estimated that of the 6.2 million estimated carers in the UK, half a million are caring for someone with a terminal illness. The majority of those people who die every year would prefer to die at home, yet only about half achieve this.
This is often due to patients unable to have their symptoms managed properly at the end of life. People often have to wait longer than what feels acceptable to them for community nurses to come and administer medications or injections. When this happens, symptoms can escalate, carers and patients can become distressed and families lose control of the situation.
Such poor management of pain relief at the end of life can lead to unplanned emergency admissions, resulting in poorer quality of life and poorer experiences for carer and dying person.
Laycarers - family, friends or people important to the dying person - tend to the individual's physical and emotional needs. They often wish they could do more, such as relieve community nursing teams of tasks like administration of medications. 39% of British adults say they would feel comfortable giving a pain-relief injection to someone who was dying and wanted to stay home, after receiving some training and with no additional support.
Current and future provision of consistent, continuous care in the community rests on laycarers being properly trained to do more. There is huge potential to 'upskill' lay carers in the practical competencies required to care and support their loved ones in the community. We believe there should be a choice for carers to be trained to give symptom control medications. It is important to note, though, that this is not an expectation, and carers must be deemed suitable by healthcare professionals.
We see the administration of medications by carers in the home, as a key element of good community care.
We seek to improve the access and quality of training and support for carers to administer subcut medications in the home. Our aim is to support patient preferences for a home death while also reducing pressure on community care teams. Our product Palliate does this by providing digital information and support via an app, to carers who have been trained to deliver medications.
Palliate closely aligns with the NHS's "Ambitions for Palliative and End of Life Care: A national framework for local action 2021-2026" by focusing on individualised, equitable care. By empowering lay-carers to administer medications for symptom relief, Palliate directly supports the ambitions of treating each person as an individual and maximising comfort and wellbeing.
Our product
Palliate, a nurse-led platform for training lay carers in the administration of end-of-life medications.
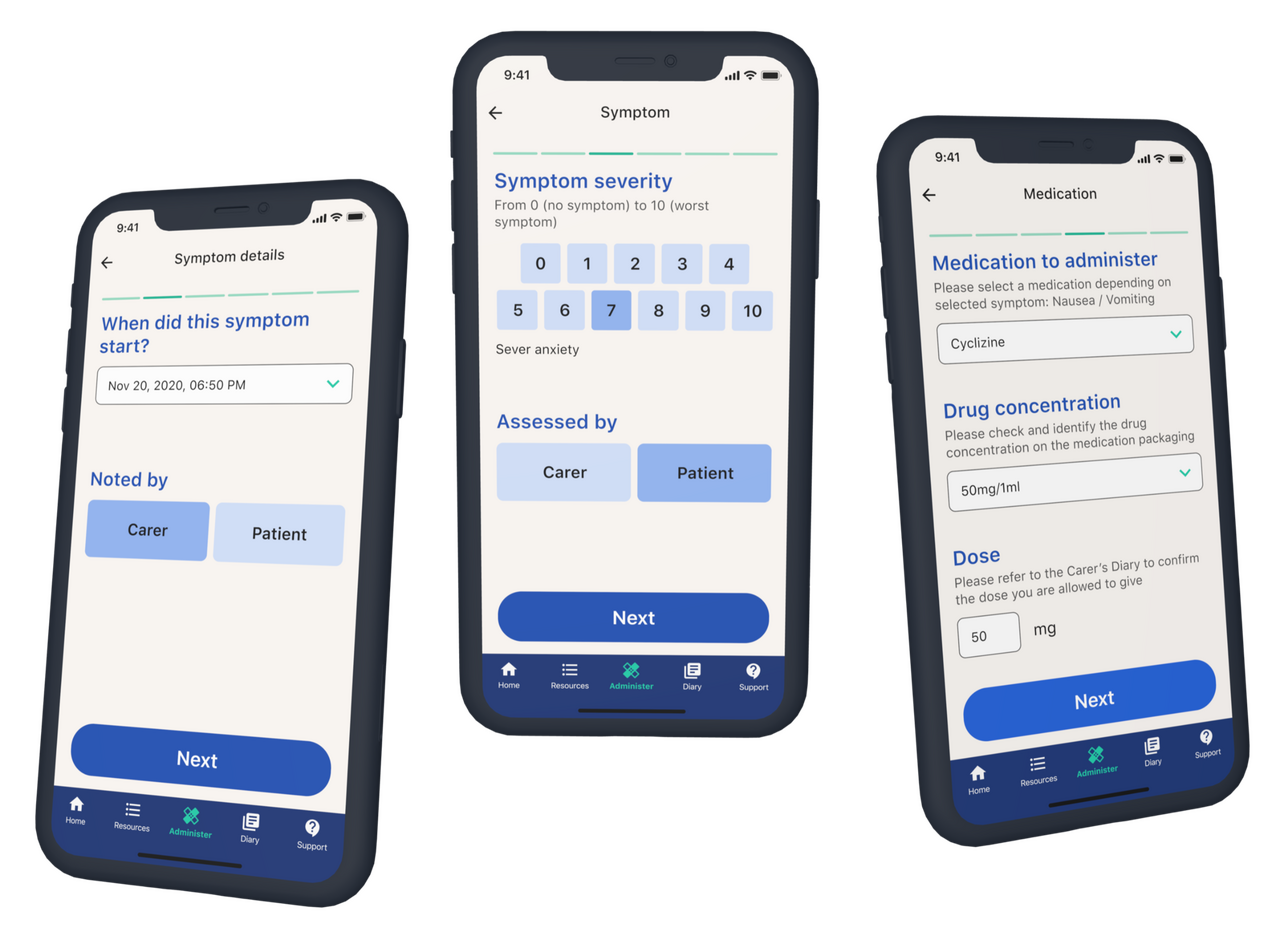
Our approach
Steps to Deliver Work:
- Initial design discovery and primary user research within clinical settings
- Accelerated development and prototyping due to COVID-19
- Design of functional digital and paper-based prototype with implementation of pre-pilot with CNWL NHS Trust
- Ongoing academic research with qualitative and quantitative studies
Users - both the public and healthcare professionals - have been integral to our development. During the COVID-19 pandemic, we collaborated with NHS England and gained invaluable feedback from frontline clinicians for our initial prototype. This laid the groundwork for our pre-pilot, where nine laycarers who were actively caring for someone at the end of life were trained using the Palliate intervention. Subsequently, we further refined Palliate features by testing additional elements like a paper preparation sheet and video-based tutorial, which were evaluated by four members of the public.
Impact so far
- Average confidence score of carers using our intervention: 8.73/10
- 91% of injections were administered without HCP assistance
- The time between symptom onset and medication administration was reduced to from over 100 minutes to 20 minutes
- Improved carer confidence was reported
- Better symptom management
Our first real-world pre-pilot, with CNWL NHS Trust, enabled patients opting for home-based palliative care, to be supported by their loved ones. One carer reported:
“I was able to improve symptoms, pain, distress, nausea….the ability to give an injection made a massive difference, most importantly for (patient) as the level of trust between us meant she wanted me to give it to her rather than other people, ie, HCP’s and this meant she was calmer as she trusted me. The short answer is that the alternative would have been calling for help and delays….the stress of someone unfamiliar always giving it to her would have made things much worse. There was no way to stop the whole thing (patient dying at home) from being stressful, but it was helpful to be in control. In some ways I felt calmer knowing and being in charge”
Next steps
- A mixed methods study to be conducted in 2024
- Further iteration and development of the Palliate product
- Piloting of the intervention in clinical environment with associated clinical studies



